WESTARM PHYSICAL THERAPY Medical Blog
Make sure that you stay up to date on the latest medical trends and treatments in the Physical Therapy realm! This medical blog is here to inform and educate our patients in their rehabilitation journey for a brighter future.


Enhancing Mobility and Range of Motion With Aquatic Therapy
In recent years, aquatic therapy has emerged as a highly effective form of treatment for individuals looking to improve their mobility and range of motion.
Vertigo and Balance Lecture – 10/24/23
Join WESTARM’s Will Jones, DPT, at the Lower Burrell facility to learn about the causes of vertigo and balance issues, what options you have for

New Aquatic Therapy Pool in Vandergrift
Check out our Vandergrift facility’s new Endless Pool, one of the most modern and spacious Aquatic Therapy pools in the Allegheny Kiski Valley area: The 90-degree heated
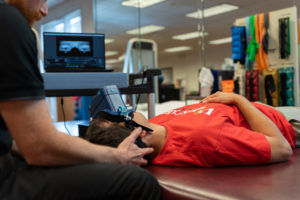
New Vertigo Treatment: Insight Infrared Video Goggles
WESTARM has obtained one of the most advanced vertigo and dizziness assessment tools on the market: the newly FDA-approved Insight Infrared Video Goggles. Vertigo is a
CELEBRATING OT MONTH WITH FUN ADAPTIVE EQUIPMENT
HAPPY OT MONTH!! Every April, we celebrate Occupational Therapy Month to honor our vital profession and the meaningful differences it makes in the lives of
WESTARM Home Health Provides Top-Notch Wound Care
Wound Care in the COVID-19 Pandemic The last year and a half have proven to be an extreme challenge for many, especially health care providers.